Celebrations | Coping | IBD | Ostomy

With Mother’s Day being yesterday, I always take time to reflect on the birth of my children. As I rocked my daughter before her nap yesterday, I cried silent tears thankful to be holding her in my arms. When my son asked to snuggle in my bed for his nap yesterday I let him just this once, and as he fell asleep on my shoulder I looked at his four year old face and could still see the baby that made me a mom. I felt lucky for these two children that call me mom, and lucky to be healthy enough to enjoy them to the fullest.
I was diagnosed with Crohn’s Disease when I was 14. For ten years I battled this disease to near death. Literal death. My health was so unstable that I was admitted to the hospital every two weeks for months. I was so dehydrated I would be on telemetry monitors for severe tachycardia. I was losing so much blood through my 30 plus bowel movements a day that I would need blood transfusions. I had a PICC line for TPN and was on total bowel rest. When I was 24, I made the decision to choose life. I was given a permanent ileostomy that gave me life. Her name is Mona the stoma.
At 27, I was told that I had hydrosalpinx in one of my fallopian tube and partially in my other tube as well when I was having irregular menstrual cycles. This was due to all the abdominal surgeries I had from my Crohn’s Disease. My OB wanted me to see a fertility specialist because she said I would have a hard time conceiving a child naturally. I declined because my partner and I weren’t ready to have children yet. Less than six weeks later, I found out I was pregnant.
My pregnancy with my son was pretty easy. I was considered high risk because of my ostomy and Crohn’s Disease. Both my GI specialist and colorectal surgeon gave the okay for a vaginal delivery. I saw a maternal fetal specialist and got a lot of ultrasounds to make sure our son was growing as he should. It was easy until 30 weeks when I developed a blockage in my intestines. I saw my ostomy nurse in the outpatient clinic and she tried to lavage my stoma with no success. With the pain getting increasingly worse I went into labor and delivery. They decided to admit me to the hospital. A doctor came in and tried to lavage the stoma again and I swear she was in my stoma all the way up to her elbow. She manipulated it so intensely that I immediately vomited and Mona immediately pooped out a pile of frosted mini wheats. They kept me in the hospital to monitor my output and monitor my baby but I narrowly avoided a NG tube and was released with the instructions to stay away from too much fiber.
Around 35 weeks I developed gestational hypertension. I was tested multiple times for preeclampsia but my urine was always clear of protein. At 37.5 weeks they decided to induce me. My colorectal surgeon was on standby if I needed a cesarean section. At 37.5 weeks with my first baby, my body was no where near ready to give birth. They started the induction with a foley bulb that helps stretch your cervix open with the intention of your body to start contracting. I wasn’t even a half centimeter dilated when we started. The foley bulb fell out around three centimeters. I was contracting so I tried to get up and walk to see if I could dilate myself more. Once the foley bulb was out and I was up walking my contractions slowed down. They introduced Pitocin to kickstart my contractions again. Around 10 hours into labor I was six centimeters dilated and opted for an epidural. After 17.5 hours of labor my contractions were coming too hard and too fast and the baby’s heart rate would drop every time I got a contraction. They had to give me a medicine to stop my contractions which made me shake involuntarily all over. At that point they started talking to me about having a cesarean. I had been in labor since 5pm the day before and it was now 10:30 am the next morning. They told me that my colorectal was ready to go and I felt an odd sense of relief that he would be there. I okayed the cesarean and they quickly wheeled me in for the emergency surgery.
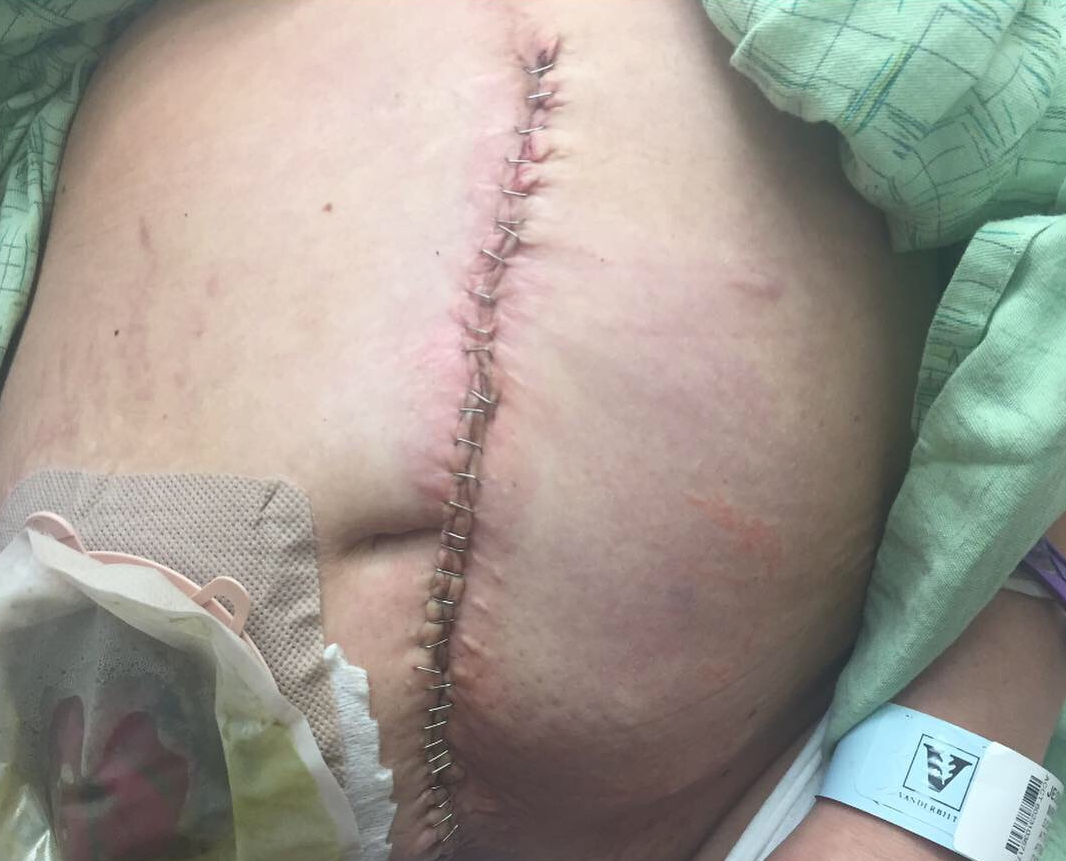
The OB that was on call had my colorectal surgeon do the incision and then the OB took over once they got to my uterus. Our son, Finnley Ellis, was born at 10:43 AM on October 2nd 2014. I remember holding him briefly and crying from the overwhelming feeling of seeing your child for the first time and the relief that he was healthy and okay. They wheeled him to the nursery with my partner never leaving his side. Because of the past abdominal surgeries they very carefully sewed me up which took much longer than it normally would. It was 12:30 before I would get to see Finn again. I was so upset that I missed that precious first hour of skin to skin where the baby is alert and is supposed to be key in starting your breastfeeding relationship. However, it turns out that you get past the early stages of breastfeeding which is not easy for a first time mom no matter what. Having that skin to skin time immediately after birth wouldn’t have made it any easier. I breastfed Finn until he was 16 months. A C-section was by far the easiest abdominal surgery recovery I had.
In October of 2016, shortly after Finnley’s second birthday, I found out I was pregnant again. This baby was as much a surprise as Finn was. I was once again considered high risk and enjoyed all the extra ultrasounds. I found out at 14 weeks that we were having a girl and I was so elated. I was also elated that the morning sickness seemed to be behind me, I was lucky to not have this particular symptom during my first pregnancy. After careful thought, we opted for a scheduled cesarean section. I would also have general surgery in the operating room to do a temporary parastomal hernia repair. We took comfort in knowing that everything could be planned out. My partners mum would be flying in from England the Friday before the June 28th C-section to take care of Finn and our pets while we were in the hospital. I even bragged at my 37 week check up that I made it through this pregnancy unscathed by any ostomy issues. At 37 weeks and six days I woke up and knew I had a blockage.
I stayed home and did all the tricks to relieve the blockage myself. I tried milking my stoma, getting in a warm bath, a warm shower, drinking hot coffee, drinking coke, I even asked on the Girls with Guts private group page what else I could do. As the day went on the pain continued to get worse. By 8pm that night, I started vomiting. I knew I needed to go to the hospital but we had no one to take care of our two year old. I remember thinking if I could just make it to 6 am we could drop him off at daycare and then we could go to the hospital. By 2am, I was vomiting every 20 minutes and in excruciating pain. I knew I couldn’t make it any longer. We called our friends in the middle of the night and took Finn to their house on the way to the hospital. I had a bucket on my lap and vomited the whole way there. I was in such extreme pain I remember struggling to even get out of the car. When we finally arrived at labor and delivery triage I was begging for them to help the pain. It felt like it took hours for them to give me an IV and give me pain medicine and nausea medicine. I was still vomiting.

My OB was luckily the OB on call that week. He came in and said “We are delivering today.” I tried to argue and say that my mother in-law wouldn’t be there until Friday and could we just wait until then. General surgery came in and made me realize that I was dangerously close to a bowel perforation which could be devastating for me and the baby. They also told me that I was going to have to be under general anesthesia because it was too dangerous for me to be awake and that my partner wouldn’t be allowed in the delivery room because they would be doing the delivery in the main operating room. I was devastated, so my OB and the anesthesia team agreed that after I had the NG tube in if I could stop vomiting they were willing to let me be awake for the delivery of our daughter and then put me under general anesthesia for the rest of the operation. I was so relieved that I wouldn’t miss the birth of my daughter. However, after they put in a NG tube I still couldn’t stop vomiting. The anesthesiologist calmly came in and told me that I was at too much of a risk for aspiration and they truly felt it was in my best interest that I be under general anesthesia the whole time. The ostomy nurse came and marked my stomach for a new stoma in case they need to operate on my intestines. I held her and cried and told her how Crohn’s was stealing this moment from me along with so much it had already taken away from me. My OB came in and said he pulled some strings and my partner could come in as long as he stayed by the incubator with the NICU team. At least her daddy would get to see her be born.
I barely remember being wheeled down to the main OR. I won’t ever forget having the catheter inserted while I was still awake, a first for me. They wanted to limit the baby’s exposure to the anesthesia so they kept me awake as long as possible. They scrubbed my stomach clean which was agonizingly painful in the state that I was already in that I was begging to just go to sleep. Sleep was a respite from the pain.
I woke up in a room alone. The nurse came in soon after as I was coming around. It looked like the same labor and delivery room I was in with my son, but my baby girl and partner weren’t there. Luckily I avoided needing any intestine removed or needing my stoma re-sited. I had to ask the nurse what time my daughter was born, how much she weighed, how long she was. When I looked at the clock on the wall it had been hours since my daughter was born. I asked when they would bring her to me. I was told that she was in the NICU at the moment and was having some blood sugar issues but as soon as her blood sugar stabilized they would bring her to me. Late that afternoon they wheeled my daughter in to my room. We did skin to skin and she tried to breastfeed but I couldn’t be left alone with her because I had been under general anesthesia. I couldn’t be trusted alone with my own baby.

On June 21st 2017, a week to the day before her scheduled cesarean section, Minnie Marie was born. It was a traumatic birth for both Minnie and I. Minnie had to be intubated for a short time after the birth because of the effects of the anesthesia. I’m told she pulled the intubation tube out on the way up to the NICU, which explains Minnie perfectly. She’s feisty and lets you know what she wants and does it her way. I still cry when I see the first photos with her and my NG tube. It took a long time to get past the hurt of Minnie’s birth and not getting to see her be born, not getting to hear her cry as she took her first breath.
As much as I feel like something was taken away from me with Minnie’s birth, I have to remember how lucky I am to have two healthy children. I wasn’t supposed to get pregnant easily or without help. Yet I did, twice. I carried those babies to term, and my body stayed healthy and free of disease so that I could breastfeed them both well past a year. Thanks to my ostomy, my body has continued to stay healthy and free of disease allowing me to care for two wild toddlers. Thanks to my ostomy I can run and walk and play with my children without being chained to a bathroom or, worse, in a hospital room.

Jessica Jay lives outside of Nashville, TN with her partner Stewart and their two children Finnley (4.5 years old) and Minnie (22 months old) and their dog and three cats. Jessica is an ostomate with Crohn’s Disease and a patient advocate. She has made a career out of having an ostomy and works in medical sales selling ostomy appliances. Her life goal is to continue to raise awareness about IBD and ostomies and to squash the stigma surrounding both.

I have uro stomy bag and cannot get bag to stick..I’m just 2 weeks out..any suggestions..Bonnie McBride